Emotional neurocircuitry . . .
. . . it’s how the brain is wired for emotions.
But in the brain of a person with PTSD, emotional distress could physically (and perhaps even visibly) change the neurocircuitry.
In a normal brain, the interaction between the hippocampus and the amygdala is important for processing emotional memory. It’s suspected that they both change in response to experience as well.
But when someone experiences trauma, do these parts of the brain change together, or are they completely independent of one another?
In a recent study led by Quan Zhang, MD at China’s Tianjin Medical University General Hospital, researchers looked at the relationship between the hippocampus and the amygdala in coal miners suffering from PTSD after surviving a gas explosion.

Specifically, they were interested in the change in gray matter volume in these areas of the brain after the traumatic experience of the blast.
Would the volume in both of these emotion-processing brain regions decrease? And if so, do the amygdala and the hippocampus change together?
Questions of how the brain changes after trauma are critical for developing more effective interventions to speed healing.
So, the researchers recruited 14 coal miners with PTSD from a gas explosion as well as a matched control group of 25 non-traumatized colleagues of the victims.
They used high-resolution magnetic resonance imaging (MRI) to look at different parts of the brain of each participant.
Then Dr. Zhang and his team used voxel-based morphometry (VBM), a computerized analysis technique to calculate brain volume from the MRIs. They looked at the differences in hippocampus and amygdala volume between the PTSD patients and the control group.
They found that the coal miners with PTSD had significantly decreased gray matter volume in the hippocampus in addition to a decrease in volume covariance between the hippocampus and amygdala compared to the control group.
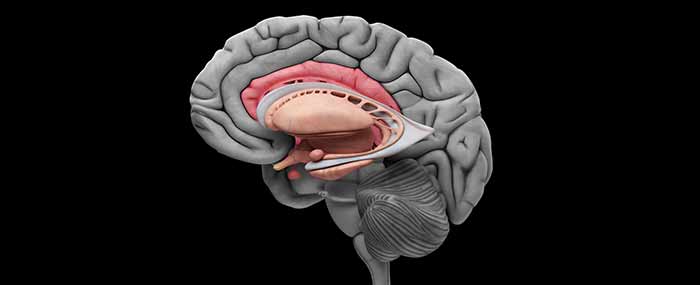
This decrease in volume may be associated with the dysfunctional emotional memory processing in PTSD patients that leads to symptoms like hyper-arousal or avoidance.
Now, we need to be careful about generalizing these findings to include all PTSD patients because the sample size was quite small. And it only included people who had been in a coal mine explosion, which means there’s a possibility some other factors could be involved.
But this work is a step toward better understanding the neurocircuitry of a brain with PTSD, which could inform our choice of intervention when working with trauma patients struggling to regulate their emotions.
If you’d like more details about Dr. Zhang’s work, these findings were published July 7, 2014 in PLOS ONE.
And if you want to learn more about how PTSD affects the brain, including some of the latest treatments that focus on rewiring the brain after trauma, then check out our Rethinking Trauma webinar series.
So now, I’d like to know what you think. Has learning about the brain impacted your work with patients who have PTSD? Please leave a comment below.
Hi!
I really enjoyed reading this and was wondering how to cite it if I wanted to use some of this information?
oavkzkpbzxvtuavhhcgyztsardeqoh
I want someone to study my brain
I am having extraordinary success along with 8 other practitioners utilizing cold laser therapy.you may download my forthcoming paper regarding case studies.go to website paintherapyusa.com
I wanted to add, this doctor seems to be doing pretty good with her understanding of helping those with PTSD. It’s really great that someone like her is working so hard to help. However, this article about emotional dysfunction, not so good. Only the part about the brain is interesting, but what happens to the brain is only the trade off for developing super human might.
PTSD should really be called, prolonged superhuman might. However, it does get more difficult to control over time as damage occurs to the body systems which overwhelmed helping with super powering the body.
PTSD after a traumatic experience is not “dysfunctional emotional processing”.
It’s really terrible that so many psychology professionals, researchers and even doctors just don’t have years of observation experience to understand that PTSD is a protection mechanism which develops in times of extreme danger. Therefore, it is NOT dysfunctional. It’s actually highly functional in order to survive danger. Understand-a person experiences extreme danger–that person becomes changed to survive extreme danger.
In those who do not develop PTSD, they are not going to survive danger as well those who do get PTSD. Therefore, those who do get it are actually more likely to survive danger, and they are stronger, faster, have faster reflexes and react much quicker to dangerous stimulus. You aren’t going to see as much of it from one traumatic experience as a war veteran who experienced extreme danger with many traumatic events for an entire year or more.
Flashbacks exist to allow for extremely fast reflexes, to bypass fear, to force an individual to spring into action, become immediately strong, fight like no other, and win at all costs, without thinking first. Get it? Flashbacks are actually NOT dysfunctional, they are highly functional taken in context of the situation.
To stop these memory imprints created to survive danger, and lower adrenaline levels in the extremely traumatized, one needs to rewrite the brain so to speak, much in the way a computer is rewritten with one operating system, in order to switch from another operating system. Make sense?
Over time, PTSD will make a person much more dysfunctional in regular everyday life, as adrenaline builds and causes damage to organ systems in the body, then making PTSD even worse. Adrenaline has been shown to kill neurons at higher levels, maybe the reason for the decrease in volume in parts of the brain? Seems likely. It also has effects on the heart, vascular system, and kidneys. It causes damage over time to keep super human powers. There is a trade off.
Please stop publishing articles on PTSD with misinformation about dysfunctional emotional processing. It’s not correct. If trauma is experienced over a long period of time, PTSD will develop, because that person’s mind has subconsciously reasoned the ability to survive future dangerous similar situations needs to be retained over a long period of time in order to survive.
I hope someone can make use of this very valuable information. There’s a saying which says, if you want the truth, get it from a child’s mouth.
“In those who do not develop PTSD, they are not going to survive danger as well those who do get PTSD. Therefore, those who do get it are actually more likely to survive danger, and they are stronger, faster, have faster reflexes and react much quicker to dangerous stimulus.”
I don’t happen to agree with you as people with PTSD don’t have the ability to evaluate situations accurately. If you’re constantly switched on to flight or flee response, you’re not likely to have the clarity of mind to make a decision as to whether a situation is actually dangerous and if so how dangerous? Sure if you have PTSD you’ll be good at fleeing but that is not always the appropriate response.So no your statement is wrong, people with PTSD might be faster at reacting to danger whether real or not, the fact that their nervous systems are on constant overdrive will mean that they will not be faster than someone without PTSD, in fact they are likely to make mistakes and die if they are in a real dangerous thought because they don’t have the benefit of a regulated nervous system that allows for clarity of thought when it matters most.
Flashbacks ARE dysfunctional because they are bit perceptions that surface that are intrusive, if they were functional super powers people with normal healthy functioning would have flashbacks all the time. They don’t and there is a reason for it.
The body is NOT geared up to be on alert all the time: it exhausts physical and mental reserves that need to be preserved for when these reserves are actually needed and put into use.
I can understand why you would want to interpret these dysfunctions as helpful super powers because feeling a sense of powerlessness when you have PTSD will mean people will grasp at any explanation to resume a sense of some control. If you have had PTSD for years you will witness your life go downhill and you feel almost powerless to change it unless you get help.
What I do marvel at is the body- mind’s rather imperfect ability to make the best of a bad situation and being gripped in absolute fear creates a scenario where brain lock occurs and then after that you’re not living you’re existing within a limited pre-programmed reflex coming from the place of fear and fear alone. How can you possibly say that is functional? Or even helpful.Scary is more like it. PTSD is about extreme dysfunction that arises from a mechanism that is meant temporarily to protect you from further harm but lands up creating more damage in the long run, if left untackled.
On the plus side there is good news.A study was conducted that suggests that a mother can trauma proof a child by ensuring that she teaches the child self regulation and self soothing.Connection and bonding teaches the child to self sooth itself.(or rather it’s teaching the nervous system a way to stay regulated and stable under all conditions)Want to make it 100% better, then try love flooding the child and this not only allows the child to feel loved and accepted but also teaches the body to release oxytocin(feel good).Oxytocin is then released that counter balances the gripping affects of fear when the person is confronting a traumatic incident. It actually then calms down the nervous system and allowing it to bounce back quickly without any permanent dysfunction or maladaptive coping mechanisms.
Try this out for size: once a day for three months, sit quietly and actually talk to yourself calmly like you would to a friend who you’re trying to reassure.Talk to yourself in a way to sooth your fears etc…. for a minimum of 30 minutes. Ensure you are deeply relaxed when you do this. I always listen to music to relax before I do this but you can do whatever gets you in a receptive state. Even if what you say to yourself doesn’t feel true: for example you can say” I feel totally and blissful safe in my body”, the aim is not so much what you say in the beginning but rather the loving calming tone of voice.At the end of the session bring up a happy memory where you were being loved and cherished with a loved one and allow that memory to expand into your body.(you can always imagine it if you have never had an experience like this) If your body is starting to feel warm and even tingly then you know you are doing it right.
So let me tell you what happens after 3 months of this: your sleep will improve massively, you will feel less days of feeling fearful for no reason and in my case, my aches and pains disappeared. I was pain free for the first time in years. In 6 months of this practise the results were even more spectacular, but don’t take my word for it, try it out yourself. This works. It’s something so simply that done continuously with practice actually re-wires the brain into being more resilient. It has been a godsend in reducing and in many cases getting rid of my PTSD symptoms all together. Obviously this is just one tool that can be used along with others.
I will have to try this. Thank you!
Thank You for these comments ;It’s encouraging coming from Children of Combat Vets. As a a Combat Vet with PTSD ; in recovery/ Renaissance for 20 years and a Presenter- Teacher in the Mental Health System , I realize that the Health care system wrongly thinks that the Brain can be Reprogramed by Chemistry and it’s functioning can be measured by the size of the Hippocampus and the number of gray mater. Chemistry can only help the brain think better ; It doesn’t tell it what to think . The brain can only be reprogramed by the Individual’s Mind as in Relearning .Learning is the original Function that Consciousness is attended by . PTSD and some other Disorders can Only be Managed by Identity Integration and ” Tibalization “.
The brain is a non-linear, complex, dynamical system and the networks of neuron synapses are constantly feeding back on each other and to many other places in the brain and body. there is no controller, coordinator. all networks feed back in many circuits leading to emergent behavior. Neurofeedback is the best intervener in that its ones own brain re-training itself using the orienting and relaxation responses built into the CNS. The Hippocampus and Amygdala are just elaborate networks that are part of the natural complex dynamical systems within the human body. Trauma can be retrained with neurofeedback as any other experience. Neurofeedback just helps whatever brain become as efficient as its structure can allow.
I think,what he was saying that if youre in combat PTSD is what keeps someone safe. Hes not saying in a persons everyday life after coming back after combat.
Everyone has their right to their own interpretations. They shouldn’t have to be told theyre,wrong for how they feel an see.
I have PTSD an have been in an out of therapy for half my life. On every medication an had Electric Shoke Treatments 12 times. An honestly nothings helped me. My fear in my conscience has never left. I would have to be brain dead to not get a trigger of some sort at anytime i see or hear of an association.
Theres nothing wrong feeling fearful an being smart. PTSD gives a 6th sense.
Isolation works for me. All people do is make judgements. Im tired of dealing with ignorant people that think i should be what society says we should be. There’s nothing wrong how i want to live my life. Im so sick an tired of having to be an do what the certain criteria is that society has made for being a person. Theres nothing wrong with being who i am an how i feel. But society says there is. I am who i am an im tired,of trying to fix myself an be someone im not to fit in. Thats the problem with the world. People have been taught to not accept one another for who they are. Everyone has a problem with one another. Its sicking an very very sad.its no wonder we have so many suicides. We’re not allowed to think we’re ok.
I hope in my next life i dont return as a human!
And i go to one of the best: DARTMOUTH
My next try will be to see if I can get Neuroplasicity if i can live that long.
I would like to be happy before I die from finding the courage to stop the misery of my life.
Part of overcoming ptsd for me was training myself to think more positively and be more appreciative of everything and everyone in life, bad and good. Because after all you are in charge of your own happiness and if you are not finding anything positive that you can focus on in your life, that’s a sign that your not as happy as you could be. And its up to you to make changes in life In ordered to find happiness. Forgive yourself and forgive others. Life is a journey and thr joy is right here around you now. You deserve a daily share of it….
I am planning to use all the new information I am learning from the Rethinking Trauma webinars with my PTSD patients and with others. I just recommended neurofeedback to a client with a son who has autism, based on what I learned in the last session. The parents have the money to follow up on this, even if insurance won’t pay for it, so she is looking for a place to get her son some neurofeedback even as I write this.
Very interesting series. Thank you.
Response to lija and anyone else interested in an excellent, readable and easy to understand guide to the different parts of the brain and their function, read “Who’s Who of the Brain – A Guide to its inhabitants, Where they live and What they do” by Prof Kenneth Nunn ISBN 978 1 84310 470 4
VERY VERY interesting – could be related to the triggering that happens so often with trauma pts
Thanx – mary
So interesting ! My mother aged 88, suffers from an unusual form of dementia. Her short-term memory and desorientation in time and place are severe. Otherwise she is not recognized as being an Alzheimer nor an age related dementia patient. The above article explains why I think… My mum is a WW2 victim, and at the age of 18 she survived bombing on her house, her mother and brother did not survive the disaster of oct26,1944. Her entire life as from that day she suffered from chronic depression, hyper arousal, avoidance as well as from schizo-affective mood swings (almost daily) and dys-functional memory processing i.e severe form of melancholia, suicidal thougts and frequent nightmares. She was/ still is a highly intelligent person. So could it be that the hippocampus underwent such a high level of stress, resulting in some form of shrinking or disactivation of packages of braincells (hubs), as a defence mechanism to “forget” the trauma ? What are your thoughts …
My thoughts are years of living with the trauma and parts of the brain could possibly stop working completely after being inactive for so long. IE: Living in a constant state of stress can reduce function especially the frontal lobe. Im no expert just diagnosed with ptsd and trying to research it myself.
Question pertaining to the above remark about “the decrease in volume (of the hippocampus & the amygdala)………… that leads to hyper-arousal or avoidance.” Does it necessarily have to be one or the other, or could it lead to both: hyper-arousal & avoidance as defense mechanisms against the fear of external imaginary threats & the fear of rejection, abandonment, etc, which in essence would all be threats to the emotional security of the person. This seems to me to be a logical deduction that both symptoms would manifest within the same time periods for many people, if not most. Thanks for the free viewing.
Aloha! This is so helpful, Ruth. The series so far has helped us understand the long-standing issues surrounding trauma, but I haven’t heard anyone address specifically childhood trauma. When an individual’s system is stressed before a sense of self develops, before the age of reason, there are unique personality development, boundary and trust issues that underlie every other learning and experience in life. I hope someone is planning to address this and share the most up-to-date treatments for what I see increasingly in my practice — Complex Post-Traumatic Stress Disorder in childhood. Thank you so much! This series will help our world tremendously. Bravo to you for hosting it!
Ruth, Seebern Fisher mentioned either the equipment she uses or the training progam but I could not understand her reference. Could you tell me what she said regarding her training.
Thank You
Yes, Sebern Fisher’s enunciation did not come through clearly at that one critical spot on the “Rethinking Trrauma…” webinar’s audio. She was referring to a product that was using a play-on-words with EEG in it’s name. ( EEGer )
Complete a web search for ” How to Conduct A Neurofeedback Session” wqhich should get you to the ” EEGer 4.3 Tutorial.” I think this will get you going.
I have noticed training days between 1 to 4 days. Contact the companies involved to learn more of the Who?, When?, Where? How long? and How much?
Hope this helps.
Further to David Berceli pointing out that trauma has been part of our evolutionary process, I’m wondering if we will also find that the body can also resolve these apparent differences post trauma ie can we track the miners years later? Will the brain differences be as apparent in 5 years time? Can the brain/body continue to heal despite stuckness and in the absence of formal therapeutic intervention? What does the body accept as health?
While we may not know specifics of trauma impact on neurocircutry, we are learning clearly that here is a physiological impact. I believe this helps reduce shame and promotes compassion and curiosity related to treating and living with the effects of trauma. I am excited about moving towards trauma informed care in many venues.
That’s a skillful answer to a dilcfiuft question
Indeed,learning more about the brain is crucial in understanding trauma. when working with PTSD I have px cortisol levels checked, so am looking forward forthe latest tx!
My name is Joe from Mass and I suffer from comlex PTSD due to birth trauma and PTSD. I am currently working with Neurofeedback 7th session today and looking to see the results over the next 7 weeks.
I find the research studies you cite difficult to trace. Could you please give more details.
Hi, this is Ricardo from Peru. I hereby send you the link to download a pdf of the study on coalminers mentioned by Ruth. Bon appetite.
Please write to my email address to confirm you have received this. Thanks for that.
Thank you for this free webinar. It’s great to be learning about the latest scientific research and the impact of trauma on the brain. I can see the use of Neurofeedback in getting the mind body connection after experiencing trauma but it sounds too technical for me. However, like all the other methods, if it works , use it. Any new knowledge is useful for adding tools to my toolbag, giving me a wider choice for intervention with individual client’s unique adaptations. There’s always some new learning in exploring new interventions even if I don’t practise the method in it’s entirety.
I wish I could get the vocabulary sorted for the different parts of the brain and their functions. It would make learning about the brain and it’s circuits so much easier. The plasticity of the brain gives us possibility for change and new learning, I find that really empowering.
Thank you for your continuing efforts to understand and explain the impact of trauma on the brain which will lead to improved treatment as we we understand brain neuroplasticity.